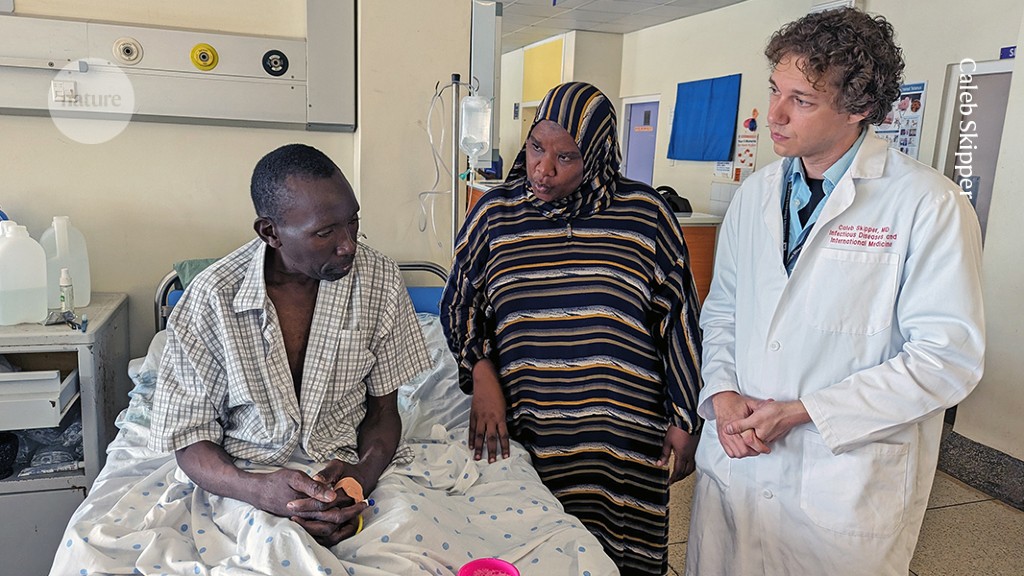
Caleb Skipper (proper) solutions questions on lumbar puncture with translation assist from Alisat Sadiq (centre) at Mulago Nationwide Referral Hospital in Kampala.Credit score: Caleb Skipper
Caleb Skipper had his first interplay with African science in 2009, when he visited Ethiopia as an undergraduate on the College of North Dakota in Grand Forks. He spent a 12 months engaged on a mission to enhance prognosis of malaria with restricted sources, which meant utilizing his instinct to improvise. For example, he helped to spice up the diagnostic capability of a well being clinic in Binishangul Gumuz, a principally rural space, by configuring a microscope that ran off solar energy. He additionally helped to implement a course of to detect malaria within the rural setting and taught native ladies the right way to work as fundamental laboratory technicians with help from a number of charities.
These early experiences confirmed him that he might work in austere circumstances and thrive in numerous cultures. They impressed him to hunt analysis alternatives with different tasks in Africa and Latin America as he pursued medical coaching.
In 2017, throughout his infectious-diseases fellowship on the College of Minnesota (UMN) in Minneapolis, he travelled to Uganda to check cytomegalovirus (CMV) as a threat think about superior HIV illness on the Infectious Ailments Institute (IDI) of Makerere College in Kampala. Throughout a 2019–20 fellowship on the IDI funded by the US Nationwide Institutes of Well being’s Fogarty Worldwide Heart, he labored on randomized medical trials of antifungal medicine and drug regimens to deal with HIV-associated cryptococcal meningitis. Now an infectious-diseases doctor on the College of Minnesota, Skipper splits his time between Minneapolis and Kampala. He tells Nature in regards to the classes he’s learnt throughout his collaborations.
How did you find yourself in Kampala?
Principally attributable to my mentors’ relationship with the IDI. Considered one of my main mentors, infectious-diseases specialist David Boulware on the UMN, has had greater than 20 years of collaboration with my different mentor, HIV and infectious-diseases specialist David Meya on the IDI. The collaboration consists of annual exchanges of medical trainees between the 2 establishments. After my preliminary expertise right here in 2017, I used to be wanting to take part in an ongoing collaboration with the IDI to broaden my information of infectious illnesses and be taught extra about the right way to ethically conduct medical analysis in resource-limited settings.
We are able to do all of the analysis right here on web site, after which the IDI owns the analysis findings. That is in distinction to amassing the information, taking it again and doing the evaluation in america after which making the native institute only a minor accomplice. The partnership is essential to constructing the native analysis capability.
How does the change programme work?
Medical college students, residents and different trainees on the UMN have alternatives to volunteer on the IDI, Makerere’s Faculty of Well being Sciences and Mulago Nationwide Referral Hospital in Kampala for periods from one month as much as one 12 months. Some volunteers principally see sufferers or educate, whereas others concentrate on analysis. I labored with David Meya and his staff, studying from their experience and observing how affected person care and medical research are carried out the IDI. Likewise, Ugandan trainees and study-team members can do medical rotations on the UMN, together with attending the UMN tropical-medicine course, and have alternatives to be taught new laboratory abilities or current analysis at conferences.
What have you ever learnt out of your expertise on the IDI, and what are you engaged on now?
I’m growing an assay on the IDI translational laboratory to detect sure viruses, equivalent to CMV and Epstein–Barr virus. I’m additionally growing improved strategies to check sufferers’ immune responses that will probably be helpful for attempting to know how viral co-infections have an effect on folks with superior HIV illness.
I’ve discovered loads by way of my time on the IDI. I’ve discovered a couple of totally different tradition, and the way that distinction can result in each fantastic moments of studying and irritating moments. For instance, to diagnose and correctly deal with folks with HIV-associated meningitis, we have to put a needle into their backbone to do a lumbar puncture to find out the reason for their meningitis. Understandably, folks could be fairly apprehensive about this. Generally they may even refuse it. It has been priceless to be taught in regards to the affected person’s perspective on why they may refuse this mandatory process, after which develop instructional supplies that would assist to handle their considerations.
I’ve additionally change into extra expert at making medical choices with out being overly reliant on diagnostic testing. And I’ve gained a greater appreciation of the dedication of caregivers and members of the family, that are issues we generally overlook in america. I hope that each one Western-trained medical doctors may have experiences in locations equivalent to Uganda to assist construct a broader and extra compassionate worldview.
On a enjoyable be aware, I’ve loved attempting new meals equivalent to a meal of matooke, the native cooked banana, eaten with groundnut paste, and studying to sail a ship on Lake Victoria.
Are you able to describe an achievement of the analysis change?
Our Ugandan staff on the IDI had a serious position in a randomized medical trial referred to as the Ambition trial, which was accomplished in 2021. The trial was for folks with HIV who develop cryptococcal meningitis, a severe fungal an infection of the mind, and the purpose was to find out whether or not a single, excessive dose of the antifungal treatment amphotericin B can be as efficient as the usual therapy, a decrease dose given over seven days and advisable by the World Well being Group (WHO). It was a multinational trial, primarily supported by the European and Growing Nations Scientific Trials Partnership, and concerned 5 African nations: Uganda, Botswana, Zimbabwe, Malawi and South Africa.
The outcomes have been printed in a 2022 examine1 led by Joe Jarvis on the London College of Hygiene & Tropical Drugs, which discovered that the single-dose amphotericin B routine was as efficient as the usual of care. As well as, the one dose was related to fewer severe adversarial occasions equivalent to anaemia and kidney damage. Owing to those findings, the WHO modified its worldwide pointers to advocate the single-dose amphotericin B routine as first-line remedy. As a result of the one dose is less complicated to manage in resource-poor settings, it can assist 1000’s of individuals residing with superior HIV worldwide to combat this lethal an infection.
This interview has been edited for size and readability.